Mackenzie
Community Health Service Area
Health Profile (Version 2.0)
Factors that affect health
The following section describes some factors that influence the health and well-being of communities. These factors act alone or in combination and impact the health of communities.
Income
Income has a substantial impact on health by affecting stress levels and other social determinants of health, such as education, living conditions (e.g., adequate housing and transportation options), and access to healthy choices (e.g., healthy food options and recreational activities).[7]
Those with the lowest levels of income are more likely to experience the poorest health, and health appears to improve with increasing income. [7] This means that all segments of the population experience the effect of income on health, not just people living in poverty.
Gross median household income in 2015
Census of population, Statistics Canada, 2016
$86,403
Education
Access to education has an impact on job opportunities, working conditions, and income level. In addition, education may contribute to greater understanding of factors and resources available that positively (or negatively) impact health. Overall, people with higher levels of education tend to be healthier than those with less formal education. [7]
Employment
Employment provides income and a sense of security for individuals. Underemployment or unemployment can lead to lower rated levels of physical and mental well-being due to factors such as reduced income that lowers the ability to make ends meet, lack of employment benefits, and elevated stress levels. Employment conditions, such as workplace safety and hours of work, can also impact health.
Employment rate (age 15+)
Census of population, Statistics Canada, 2016
65%
Housing Stability
People with unsuitable, unaffordable, or inadequate housing are more likely to experience unstable housing, such as moving frequently, living in shelters, or staying with friends or family.[6] Moving often can be unsettling and have a large impact on wellness, especially on mental health.[8]
Data source: Census of population, Statistics Canada, 2016
Community Belonging and Loneliness
People's sense of belonging to their local community relates to their social engagement and participation within their community.[9] Research has shown that social engagement and a strong sense of community belonging are associated with positive health outcomes.[10] Social engagement and community belonging are also linked to improved physical and mental health, even when influential factors such as age and sex are taken into account.[9,11] Loneliness, on the other hand, is shown to be associated with poorer physical and mental health outcomes,[12, 13] a particular concern for the elderly and frail who live alone.
Local and Indigenous governments, community organizations, and health authorities can promote social engagement and peoples' belongingness to their communities by supporting or providing a variety of social programming.
Prepared by BC Centere for Disease Control.
Prepared by BC Centere for Disease Control.
Sociodemographic diversity
People may have different experiences accessing resources based on their gender, race, age, ethnicity, language spoken, etc., which can shape their material and social circumstances. In turn, people’s health and well-being are influenced by the dynamic interplay between many factors, including where they live and work, their demographic and socioeconomic characteristics, and other social and material elements.[14,15,16]
By capturing the geographic, demographic, and socioeconomic factors known to be important to health equity, the British Columbia Index of Multiple Deprivation (BCIMD) provides a summary measure for each CHSA that can reflect the sociodemographic diversity and inequities that exist in these complex systems.[17]
The BCIMD comprises four dimensions: residential instability, economic dependency, ethno-cultural composition, and situational vulnerability. Within a dimension, each CHSA receives a score. The scores for all CHSAs are then ordered based on the number value and categorized into five groups or quintiles.
Quintile 1 of the index represents the least deprived (or least diverse), and quintile 5 represents the most deprived/diverse CHSA in each dimension. This way, distinctive characteristics of a community can be captured using the BCIMD, where a given CHSA may have a high quintile ranking in one dimension and a low quintile ranking in another.
Quintile 1 of the index represents the least deprived (or least ethno-culturally diverse), and quintile 5 represents the most deprived/diverse in each dimension.
Data source: BC Centre for Disease Control. (2022). BC's Index of Multiple Deprivation for Community Health Service Areas. Prepared by BC Centre for Disease Control.
Area-based socioeconomic indicators, such as the BCIMD, are population-level metrics. While they do not necessarily represent the experience of individuals, they can be and have been used to inform strategies to improve patient care and public health services at the community level.
Situational vulnerability
Situational vulnerability refers to differences in sociodemographic conditions or factors including housing and education. The indicators included in this dimension measure concepts such as the proportion of population that identifies as Indigenous, the proportion of population aged 25-64 without a high school diploma, the proportion of dwellings needing major repairs, the proportion of population that is low-income, and the proportion of single parent families.
Ethno-cultural composition
Ethno-cultural composition refers to the ethnic and cultural diversity within a community. The indicators included in this dimension measure concepts such as the proportion of population who self-identify as a visible minority, the proportion of population that is foreign-born, the proportion of population who are recent immigrants, and the proportion of population who are linguistically isolated (have no knowledge of either official languages).
Economic dependency
Economic dependency refers to the household dependency on the workforce or on other sources of income. The indicators included in this dimension measure concepts such as the proportion of population participating in the labour force, the proportion of population aged 65 and older, the ratio of employment to population, and the dependency ratio (the population aged 0-14 years and aged 65 years and older divided by the population aged 15-64 years).
Residential instability
Residential instability refers to the tendency of people who live in their neighbourhood to change their place of residence over time, while considering characteristics such as housing and family. The indicators included in this dimension measure concepts such as the proportions of dwellings that are apartment buildings, the proportion of people living alone, the proportion of dwellings that are owned, and the proportion of population who moved within the last five years.
Built Environment
The built (or physical) environment can promote healthy behaviours and reduce injuries by reducing environmental hazards and/or increasing access to healthy food outlets, affordable safe housing, safe and accessible transportation systems, recreational spaces, and opportunities for social connectedness. A community's built environment determines which healthy and safe options are available, affordable, and accessible for everyone.
Local communities can create healthier built environments for residents by integrating health and access to physical activity into planning and policy activities.
Active Living Environment
Built environments support physical activity in daily life through walking, cycling, and using public transportation. The Canadian Active Living Environments (Can-ALE) database provides a set of measures that represent the active living friendliness, or “walkability”, of neighbourhoods.[18] In the map shown below, “least” means the dissemination area (DA) is least favourable to active living and “most” means the area is most favourable to active living. [18]
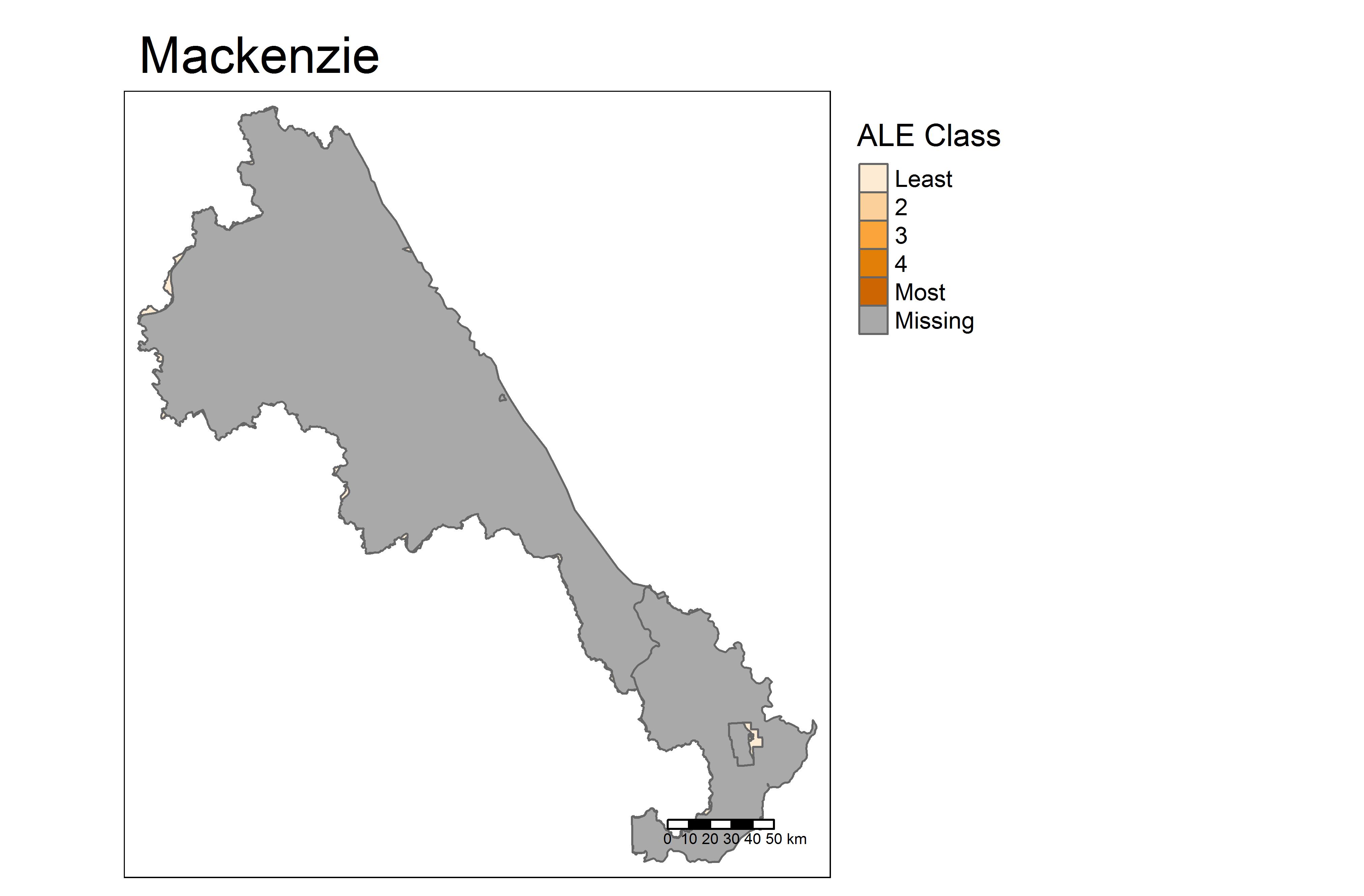
Dissemination Area: A dissemination area (DA) is a small, relatively stable geographic unit composed of one or more adjacent dissemination blocks with an average population of 400 to 700 persons based on data from the previous Census of Population Program. Dissemination areas are the smallest standard geographic areas for which all census data are disseminated. Each CHSA includes several dissemination areas.
(Census of population, Statistics Canada, 2016)
Climate change
Climate change is affecting the health and well-being of communities in BC, and these impacts will continue in the decades ahead. Climate change can affect health and well-being directly and indirectly and on different timelines.
People across the province of BC may be impacted differently. The effects of climate change vary in different locations. Some areas are experiencing faster warming, some are experiencing more wildfires and droughts, and some are experiencing more storm surges and sea level rise. Some people and communities are also more susceptible to the health impacts of climate change. Factors that increase risk include lower income, less social support, disabilities, older age, chronic diseases, and mental illnesses.[19] Work is currently underway in BC to develop indicators of community susceptibility to different climatic changes. Until this work is complete, there is existing information that communities can use to understand their climate risks.
For information about how climate change may impact your community, visit climatedata.ca.
To access other climate change resources for British Columbians, visit Plan2Adapt from the Pacific Climate Impacts Consortium.

